
Mechanical low back pain is an emerging problem. The term ‘mechanical’ refers to the fact that the vertebral column receives physical forces that destroy the soft tissues, resulting in pain and uncomfortable sensations.
The mobile parts of the vertebral column include muscles, tendons, ligaments, vertebral bodies, facet joints, intervertebral discs, as well as surrounding soft tissues. The motion of these mobile parts triggers mechanical pain.
The lumbar region of the vertebral column is a common region for the occurrence of mechanical back pain because all the five lumbar vertebrae absorb and distribute a major portion of the body weight during movements and rest.
The neck is also a common region for mechanical pain to occur, as it is the most mobile part of the vertebral column. It contains seven cervical vertebrae which support the head and are much smaller than the lumbar vertebrae.
A vast range of motions takes place at neck including bending forward, nodding, bending backward and side to side.
A back or neck sprain usually takes place when ligaments of the vertebral column are overstretched or torn. Neck or back sprain may also occur due to the involvement of muscles and tendons. Due to injury, muscles of affected part go into a spasm which causes severe pain and stiffness while moving.
Mechanical lower back pain (or mechanica pain in general) is a type of back pain that is contrasting to inflammatory back pain (or simply inflammatory pain) – which covers spinal conditions such as spondyloarthritis, which includes issues such as ankylosing spondylitis or inflammatory arthritis.
As we have already discussed, mechanical back pain is mostly triggered by injuries or spasms of muscles and other soft tissues. Here we’ll discuss some other conditions which cause pain in your back while moving.
Intervertebral discs are present between each adjacent vertebrae. Each disc contains two parts – an outer ring-like structure called ‘annulus fibrosus’ and inner jelly-like material called ‘nucleus pulposus’. When the inner jelly-like material comes out of the outer ring due to an injury or trauma, the condition is known as disc herniation.
A vertebral compression fracture takes place when a vertebral body collapses. A vertebral compression fracture may take place due to trauma or osteoporosis, a degenerative bone disease in which bones become weakened and prone to injury.
In the patients with osteoporosis, a vertebral compression fracture may happen spontaneously during routine movements like bending forward or lifting a heavy weight. These fractures cause pain which is sudden in onset and severe in nature.
Spinal stenosis is a condition where the spinal canal or the passageways of nerve roots become narrowed. Due to this narrowing, nerves become compressed and pain is the first symptom to be felt. This pain can radiate to arms, legs, and feet. When it radiates to the buttocks and one or both legs, it is termed as sciatica.
Lumbar spinal stenosis occurs due to degenerative disc disease and is most common in old age. One reason for this is due to bony spurs that usually grow in the old age patients of spinal stenosis, so nerves are pressed due to less available space.
It is also termed ‘spondylosis’, and it is a degenerative disease of the vertebral column. Spondylosis can affect the facet joints of the vertebral column, causing stiffness, swelling, and pain. It can occur in any area of the back including the neck, the middle part of the back (thoracic region) and lower back (lumbar region). When it affects the lower region of the back, it can be referred to as ‘lumbar spondylosis’.
Below we’ll describe some of the risk factors associated with the development of mechanical back pain. Typical risk factors include:
Wear and tear changes occur in the vertebral column with advancing age, which leads to certain conditions that we have already discussed above like spinal osteoarthritis, spinal canal stenosis and bony spurs, etc. These conditions produce chronic neck and back pain. People between the age of thirty to sixty years are more prone to develop disc-related disorders while people above the age of sixty years have more chances of developing osteoarthritis.
Certain kinds of vertebral column disorders have a genetic component. An example can be given in terms of degenerative disc disease, which has an inherited component.
Any type of job which demands repetitive bending movements and heavy weight lifting has a high prevalence of developing back pain (e.g. nurses, surgeons, construction workers, manual labourers).
Jobs that demand prolonged periods of standing, e.g. barbers, hairdressers, chefs etc.
On the other hand, people who work in jobs that require long periods of sitting, such as software developers and accountants, also put the people in the category of high-risk people. This is so because the back is not supported at all for prolonged periods of time.
Lack of physical activity and regular exercise enhances the likelihood of chronic low back pain to develop and also increases the severity of pain.
Extra weight puts extra pressure to the muscles of the back, as well as on the bones of the spinal column, which are thus strained. Being overweight also enhances the risk of knee and other joints pain.
Any kind of poor posture that is maintained for a prolonged period of time significantly enhances the risk for chronic back pain.
Mechanical back pain is treated in the same way as other kinds of back pains. Treatment modalities include non-surgical approaches (bed rest, painkillers and supervised therapy programs) and surgical interventions if needed.
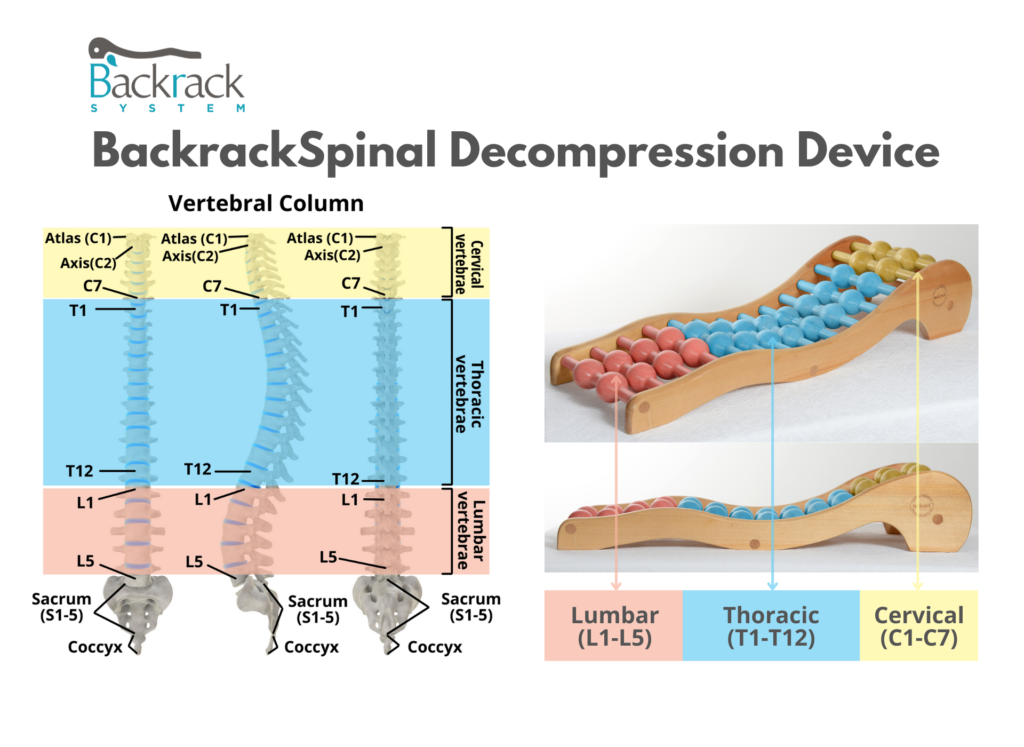
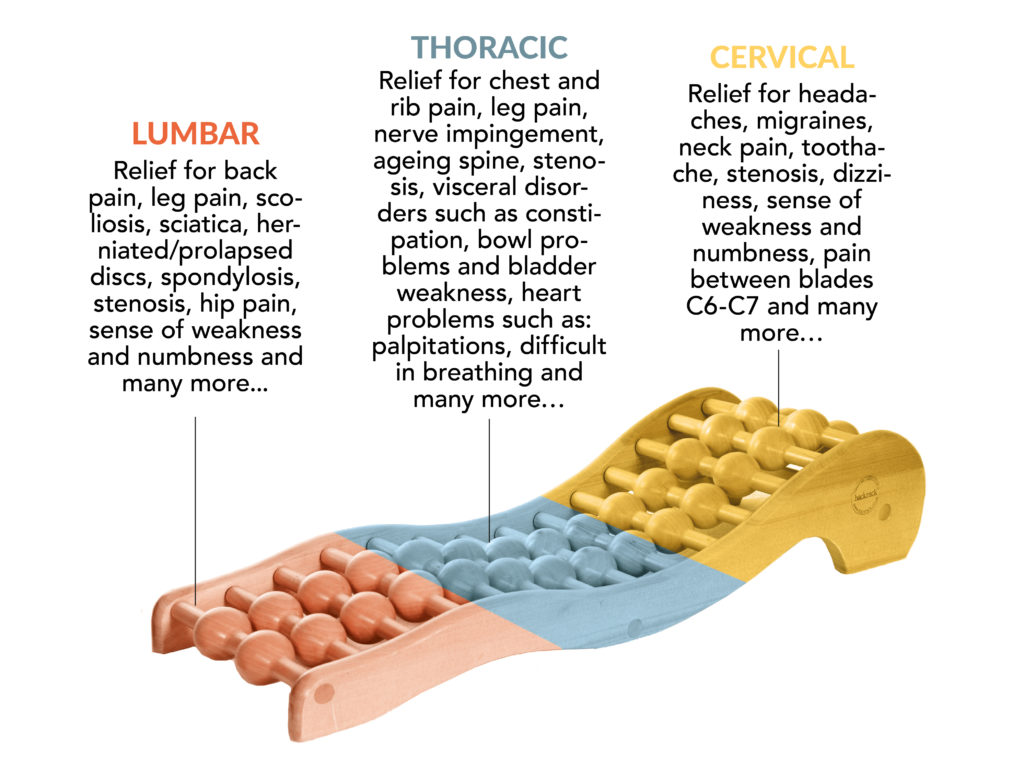
Add Backrack™ to your daily lifestyle to treat and prevent all forms of Back pain and their associated symptoms. It is truly a stand-alone product in back care.
Short-term bed rest is suggested for patients who suffer from back pain due to muscle spasms. Bed rest of greater than 45 to 48 hours is generally not recommended.
Applying hot or cold fomentation is helpful for reducing inflammation and pain. Cold fomentations improve blood supply, which is good for spinal issues.
It is usually recommended that you apply hot fomentation for 20 minutes and then cold compress for 20 minutes. You can apply each compress individually. Apply each compress 2 to 3 times a day.
Author: Spinal Backrack
Sign up our newsletter to get article update about backrack therapy.
Unsure which protocol you need? Select your symptoms for a clinical recommendation.