
If you have deep buttock pain that feels sharp, burning, aching, or like an electric shock, you might be dealing with sciatica or something that closely mimics it. People often notice it most when sitting, getting out of the car, bending forward, or after a long day on their feet.
This guide answers the question what causes sciatica buttock pain and helps you narrow down what is most likely in your case. You will also find practical, safe at-home steps that many people use to calm symptoms and support recovery.
Important note: This article is educational and not medical advice. If you have severe symptoms, symptoms that are getting worse, or any red flags listed below, get evaluated by a qualified healthcare professional.
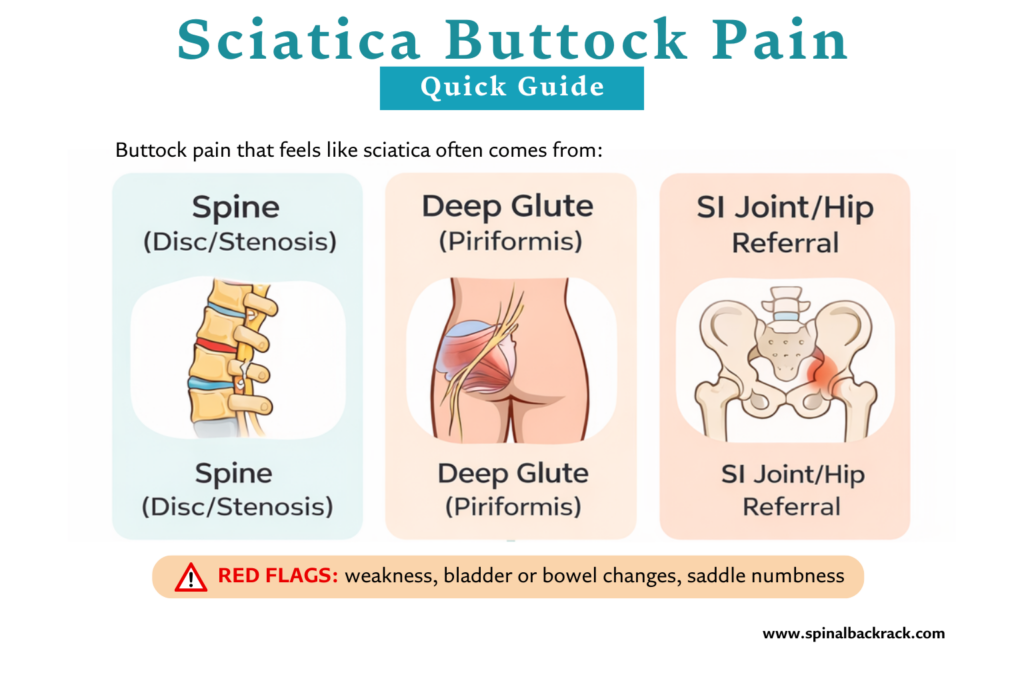
Sciatica is a set of symptoms that usually happens when one or more nerve roots in the lower spine become irritated or compressed, most commonly around L4 to S1. The sciatic nerve is the large nerve that runs from the lower back through the buttock and down the back of the leg. When the nerve pathway is irritated, pain can show up in the buttock, then travel into the thigh, calf, or foot.
Two important things to know:
That is why identifying the most likely cause matters.
Below are the most common causes and mimics. Each one includes a typical pattern, common triggers, and what often helps.
Typical pattern
Common triggers
What often helps
If you are not sure whether your symptoms are sciatica or general low back pain, read our guide on lower back pain vs sciatica.
Typical pattern
Common triggers
What often helps
Typical pattern
Common triggers
What often helps
Learn how to tell the difference in our guide on sciatica vs piriformis syndrome.
Typical pattern
Common triggers
What often helps
Typical pattern
Common triggers
What often helps
Typical pattern
Common triggers
What often helps
For sitting-related pain, see buttock pain when sitting could be sciatica.
Typical pattern
Common triggers
What often helps
Typical pattern
Common triggers
What often helps
Most sciatica-like buttock pain is mechanical, but some causes require medical evaluation.
Examples include:
If you see red flags, do not rely on internet advice.
See what conditions that can be mistaken for sciatica.
Sitting increases pressure through the discs and can place the lower spine in a flexed position. For many people, that combination can aggravate a disc-related sciatica pattern. Sitting can also compress structures in the deep glute area, which can aggravate piriformis or deep gluteal syndrome. That is why sitting-related buttock pain can have more than one source.
A useful clue is what happens when you change positions:
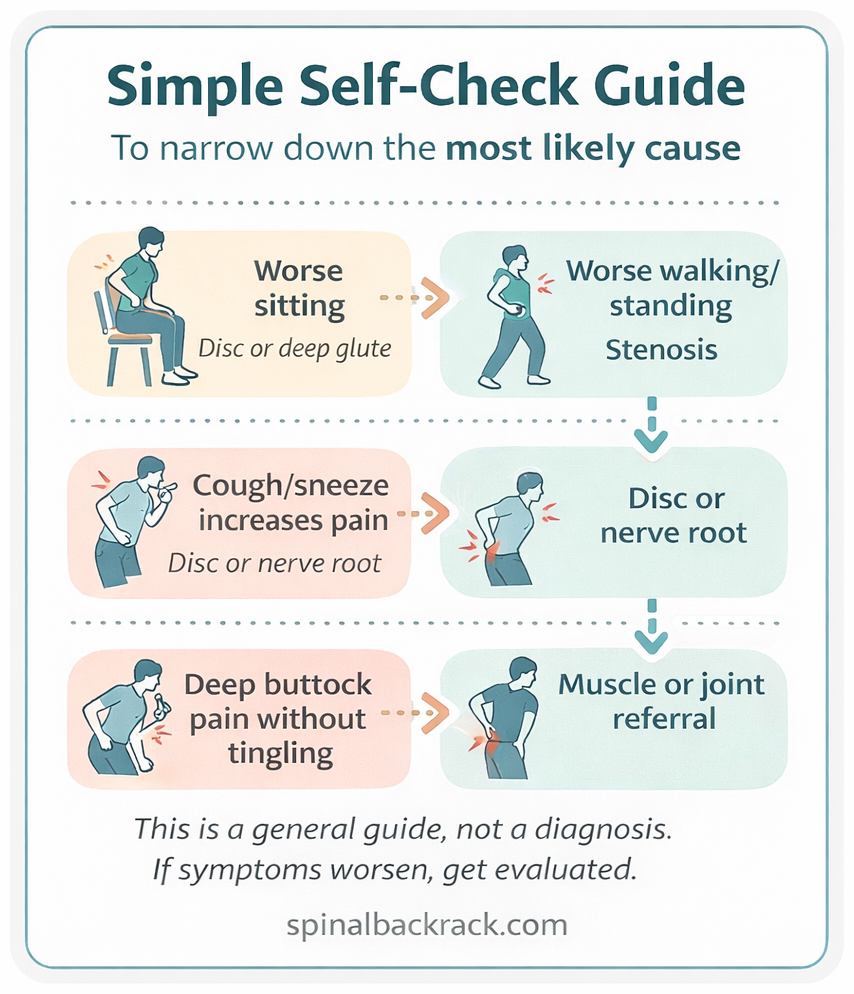
This is not a diagnosis. It is a practical way to organize patterns so you can choose safer next steps.
Most likely patterns:
Next step:
Most likely pattern:
Next step:
Most likely pattern:
Next step:
More likely patterns:
Next step:
Seek urgent medical care if you have any of the following:
These steps are conservative and focus on reducing irritation and building tolerance.
If a movement or position reliably spikes symptoms, reduce it temporarily. The goal is not to avoid movement forever. The goal is to calm the irritation so you can rebuild.
Examples:
Many people do best with a simple rule:
Even 2 to 5 minutes of walking or gentle movement can reduce symptoms for the next hour.
The idea is to reduce pressure and allow the nervous system to relax.
Options that many people tolerate:
Stop if symptoms sharply worsen or strongly radiate farther down the leg.
Walking is often helpful because it improves circulation, reduces stiffness, and supports recovery. Keep it short and repeatable.
If walking worsens symptoms quickly, shift toward shorter bouts and more frequent breaks.
Think in terms of low-intensity consistency.
If night pain is an issue:
Many causes of sciatica-like buttock pain involve a combination of compression, stiffness, and sensitivity in the low back and hips. For people who respond well to gentle unloading, a consistent at-home routine can be a useful part of the solution.
Backrack is designed to support a simple decompression-style routine at home. The best way to use a tool like this is not to chase intensity, but to build consistency.
Most readers start with the Backrack device. The combo is optional for people who want added lumbar support.


Tap an option to view details and variations.
Talk with a qualified clinician first if you have:
Common mimics include piriformis or deep gluteal syndrome, SI joint referral, hip joint issues, and trigger points.
Yes. It can start in the buttock and show minimal back pain, especially when the primary irritation is the nerve pathway rather than the back muscles. It can also be a mimic like piriformis syndrome or SI joint referral.
Sitting can increase disc pressure and place the lower spine in a position that irritates nerve roots. It can also compress deep glute structures that can irritate the sciatic nerve pathway.
It varies widely. Some flares settle in days to weeks with conservative care and better loading habits. If symptoms persist, worsen, or include weakness, it is worth getting evaluated.
Gentle stretching can help some people, but aggressive deep stretching can worsen symptoms when the nerve is irritated. Start gently and stop if the pain sharply radiates or intensifies.
The best choices depend on the cause, but many people do well with:
If any exercise increases sharp radiating pain, scale it back.
Common mimics include piriformis or deep gluteal syndrome, SI joint referral, hip joint issues, and trigger points. Internal reading suggestion: link to your post using anchor text like conditions mistaken for sciatica.
If you want a straightforward starting plan, do this for 7 days:
If you are still asking what causes sciatica buttock pain, start with the patterns and steps above and consider a gentle decompression routine you can do consistently.


Sign up our newsletter to get article update about backrack therapy.